Port St Lucie, FL
Welcome to Kelly’s Animal Hospital
We are Port St. Lucie’s premier animal hospital since 1992. We strive to offer the best and most affordable, quality pet care.

It’s official! Thanks to our people, we’re proud to have earned Great Place to Work® Certification™. Our company culture is our top priority! #GPTWcertified
OUR VETERINARY SERVICES
We Are A Full-Service Pet Hospital
Kelly’s Animal Hospital offers the following veterinary services for dogs and cats of all breeds, ages, medical conditions, and lifestyles:
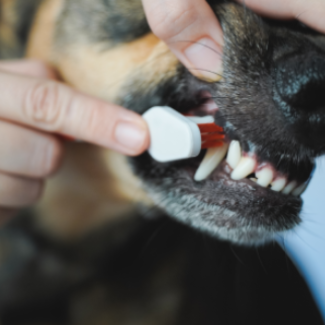
Pet Dental
Our practice requires anesthesia for dental procedures. Because of this, we first perform a full physical exam and sometimes run blood tests.
Pet Boarding
Each pet gets plenty of physical exercise, fresh air, and sunlight. Our practice hosts social playtime in small groups or you can ask that we walk your pet individually.
Pet Surgery
Elective procedures are carried out when your pet is generally regarded as healthy, significantly lowering
the likelihood of complications.
Call Us For Our
Latest Promotions
STATE VETERINARY MEDICAL ASSOCIATIONS
We Proudly Serve The Pets Of Port St. Lucie, Florida
Kelly’s Animal Hospital has extensive training in the management of pet health issues. We are a full-service facility with a friendly veterinary team. We look forward to meeting you soon!




OUR STORY
Welcome To Kelly’s Animal Hospital
We look forward to serving you and your pet with the best possible veterinary care. We utilize the most current standards of care, and we specialize in providing comprehensive wellness care to keep your pet healthy throughout their long and happy life.
THEY LOVE US
Thank You For All Your Kind Words.

OUR VETERINARY TEAM
Meet Our Skilled Team
At Kelly’s Animal Hospital, our veterinary staff will take the time required to offer the most competent care possible while utilizing cutting-edge techniques. We treat your pets with the same compassion and decency we would our own, providing the best care possible.